Current Update on Fungal Nail Biofilms 2025
Compleet Feet drew the public’s attention to the ‘Super Fungus’ in 2017. Fungal Nail (onychomycosis) was demonstrating treatment resistance to conventional methods. We are aware of bacterial antibiotic resistance, but there is less understanding regarding the ineffectiveness of antifungal agents on mycotic infections affecting the body e.g nail fungus.
As with antibiotic resistance the main reason antibiotics fail is due to the presence of a biofilm. A microscopic impenetrable barrier. This ‘barrier’ biofilm can form within the lower layers of the nail plate. Fungal biofilms are a coalescence of fungal cells, forming a complex microscopic impenetrable matrix within the nail plate. The matrix becomes very organised with polysaccharides, proteins, lipids, and extracellular DNA. These biofilms attach firmly to surfaces such as the nail plate (keratin), and protect the fungus from antifungal agents and immune defences. Applying a topical antifungal formulation to the nail is pointless. Taking oral medication too can be ineffective. The reasons why, are almost science fiction. The baddies (dermophytes) will do anything to survive. All that the body’s immune system does to protect itself from unwanted ‘invaders’, is challenged. Everything is turned upside on its head.

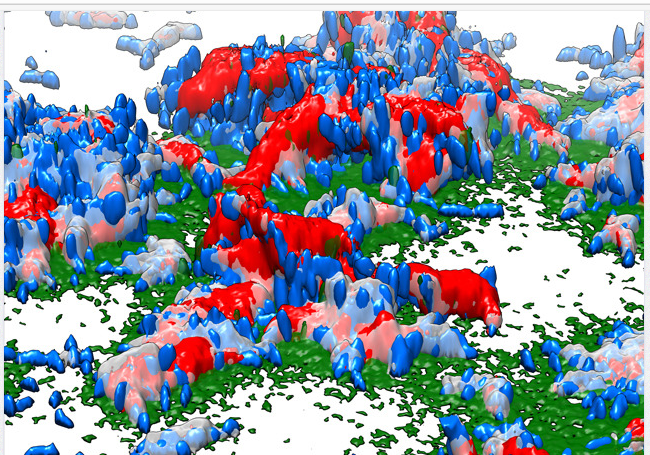
Fungal Nail Biofilm Deep Within an Infected Nail Plate

Microscopic image of a fungal biofilm within the nail plate.
How The Nail Fungus Resists Treatments
- Forms a biofilm barrier effect of the matrix acting like an impenetrable shield
- Alters metabolic activity, whereby trapped fungal spores, dermophytes are inactive or slow growing. Drugs aim to target actively dividing cells.
- Upregulates action of Efflux pumps. These are cellular defence mechanisms which literally pump, out the antifungal drugs to protect the toxic nasties within the matrix. Us versus them scenario.

The infected fungal cell has a pump to expel the antifungal drug rendering them ineffective
- Stresses the immune system. Stress response genes stay chronically upregulated. This means there is a constant low-level inflammation which is not good for cells, but is great for fungus. Keeps the fungus in a heightened survival mode, permanently fighting against antifungal agents.
- Dormant, stealth Persister cells. A small subpopulation of dormant cells ( hibernating spores) which can survive everything thrown at them and repopulate the biofilm once treatment stops. They are identical to the other fungal cells, but go into a ‘sleep mode’; under the radar to evade a drug’s effect. Persister cells are abundant in fungal biofilms. They tend to cluster deeply together. A dermatophytoma contains a high concentration of persister cells.

Note the presence of a couple of treatment resistant fungal bodies within the infection group.
- Gene expression changes to fungal cellular walls. In a retaliation to external threats(drugs), the infected cells remodel their walls by switching on their efflux pumps and altering target enzymes to make the walls stronger.
- The clinical implications for a podiatrist treating a chronic fungal infection is that they have a very challenging battle ahead. The efficacy of standard drugs e.g. Terbinafine, Itraconazole, and Fluconazole are less effective. Re-infection rates high. Prolonged over-use of drugs can increase toxicity risks. Hepatic issues.
Diagnosing the presence of a biofilm?
Routine cultures or microscopy often miss the structured embedded infection, therefor the experience of a podiatrist is crucial as a diagnostic tool. Good history taking is the key:
- Observing fungal infections not responding to treatments
- Reoccurring infections
- Localised dense streaks or patches e.g. dermatophytomas
- Poor drug penetration
- Quality of nail bed getting increasingly worse or more occluded
- The length of time the infection has been present
- Other infected family members with treatment resistant infections.
Fungal Nail Treatment Resistance can be Inherited
Research is revealing, that if a person has sustained a long exposure to their fungal nail infection, epigenic gene changes can occur. Their infection is locked in resistance; thus, the fungus permanently expresses a “resistant phenotype”. This resistance to fight nail fungus can be inherited. Anecdotally, this writer has noted an increase in children under the age of 5 having treatment resistant infections.
A Challenging Good Versus Bad Scenario
Once a potential fungal biofilm has been diagnosed the battle begins. A multi-disciplined approach is required to achieve an efficacious gaol. The more the clinician and patient can throw at throw at the infection the more chances of winning. There are 3 main cycles of infection which need to be broken. It is imperative to eradicate all persister cells (spores). The most effective way to eradicate a biofilm is to surgically remove it. Simply debriding, reducing the thickness of the infected nail can be ineffective. Any trace of the biofilm left behind will lead to it reforming its battle shield matrix. It all has to go, and then the nail bed and surrounding structures treated for the presence of any remaining fungal elements. Photodynamic therapy; Lunula laser therapy is a powerful adjunctive weapon to utilise in the ‘battle’.
Breaking the 3 Cycles of Fungal Nail Infection
- Nails -Removal/ treatment of infected nails.
- Skin – Eradication of any Athletes Foot (tinea pedis). Anti-fungal creams, drugs
- External – Decontamination of footwear and socks e.g, throwing away old shoes/slippers

Important to break all cycles of infection or risk re-infection
It is role of the podiatrist to empower the patient and give them the right mindset and tools to eradicate their fungal nail infection. Patience and determination is required. Unfortunately, there are some cases whereby the ‘Super Fungus persists. The patient may have a treatment ‘resistant phenotype. The infection is locked in. In these cases, we just have to work harder, or suggest that it may be prudent to phenolise the diseased nail matrix. This will prevent the nail re-growing. The health of the patient has to be considered. Having the presence of a low- grade fungal infection can raise unwanted inflammatory markers within the body. The body is constantly trying to fight it, thus when it weakened e.g. stress, aging, the nail fungus as an opportunist can spread to infect other nails.
CONCLUSION Act Quickly!
The quicker an individual acts if they suspect they have a fungal nail infection (onychomycosis), the better the outcome. Seek help and advice and start treating the disease. Having fungal nails can seriously affect your mental and physical health.
This author asked ChatGPT if there are any advancements in the treatment of fungal biofilm?
🧪 Emerging strategies to combat biofilm resistance 13-10-2025
- Biofilm-disrupting agents:
- Enzymes (e.g., DNase, proteases, dispersin B) to degrade the ECM.
- Surfactants or chelating agents to destabilize the matrix.
- Novel drug delivery systems:
- Nanoparticles, liposomes, and hydrogels can improve drug penetration.
- Iontophoresis and laser-assisted delivery can enhance drug uptake through the nail plate.
- Combination therapy:
- Topical + systemic antifungal combinations may be more effective.
- Synergistic combinations with antibiofilm agents are under investigation.
- Photodynamic therapy and lasers:
- These physically disrupt biofilms and kill embedded fungal cells.
- Natural compounds:
- Plant-derived agents (e.g., thymol, eugenol, tea tree oil) show some antibiofilm activity in vitro.