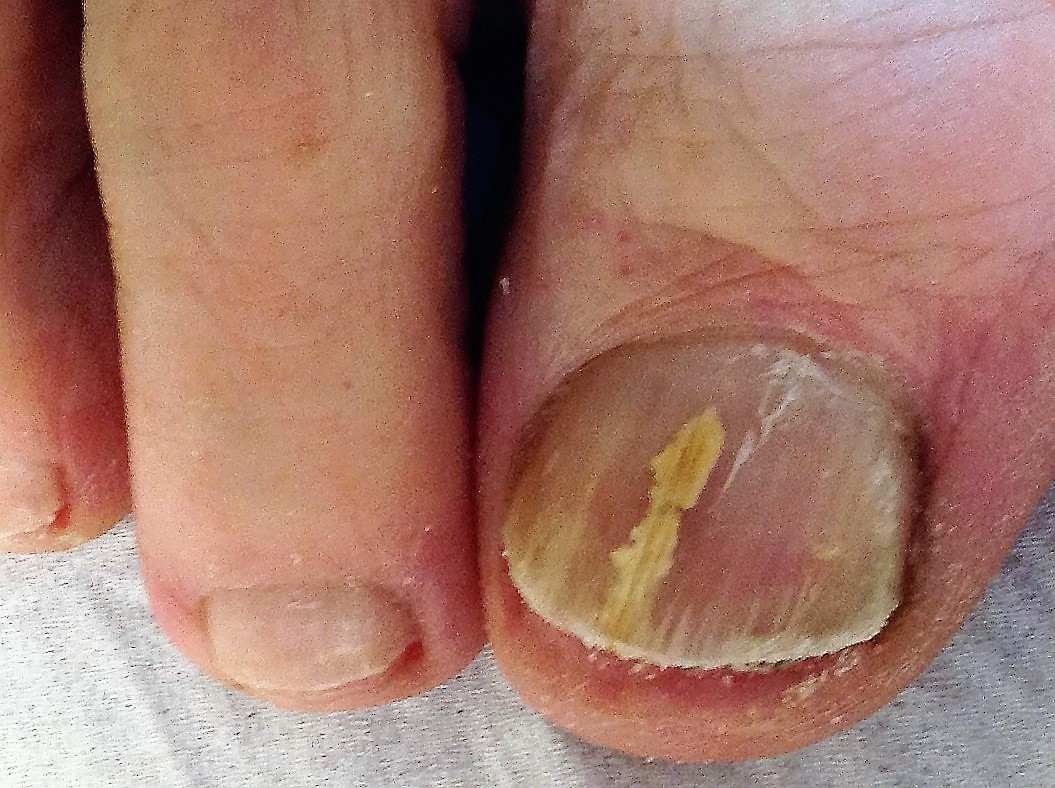
There are often cases whereby we get patients who have what appears just to be a simple streak of fungal nail infection that just does not respond easily to treatment. Yellow streaks of discolouration which suddenly appear from nowhere, but continue at a pace to race forwards the nail matrix. Antifungal topical preparations have zero effect, and what should be considered a low-grade infection requiring the minimum of just 4 Lunula laser treatments requires 8 which is normally resolved for a high grade long standing infection. Why is this?
It is so easy to lump all fungal nail infections into the onychomycosis bracket, but not all infections are the same. In 1998 Jones and Evans identified the dermatophytoma which is not commonly discussed in UK podiatry onychomycosis literature. A dermatophytoma is characterised by the appearance of a yellow longitudinal streak extending from the free edge of a nail plate spiking inwards. They can also appear as yellow patches appearing in the centre of a nail plate. The fungal dermaphytes create a thick fungal mass within and under the nail plate which is especially resistant to treatment. Dermatophytomas have a dense fungal framework and composition made up of hyphae filaments and keratin debris. Microscopically infected cell walls are thickened and abnormal.
Dermatophytomas are resistant to most topical drugs. It is hard for the active ingredients to be absorbed into the densely compacted composition. The effectiveness of drug absorption into nail plates is generally low. Nail plates are like plywood consisting of many layers, and the actual infection is harboured in layers close to the nail bed. The drug needs to penetrate through all the layers. The Clearanail treatment can increase drug efficacy. This micro-penetration drill can painlessly introduce multiple minute holes into the nail plate to allow absorption of terbinafine hydrochloride molecules into site of infection. Usually only one treatment session is required, but with the presence of a dermatophytoma often several sessions are required, in what just seems to be a minor low-grade infection.

To complicate the difficulties in effectively treating dermatophytomas there may be the presence of a biofilm. Biofilms are populations of micro-organisms that adhere to surfaces and produce an extracellular polysaccharide barrier. Biofilms have been associated with approximately 80% of all human infections. Detection is extremely difficult with routine culture techniques. Biofilms can be resistant to standard antimicrobials and antifungal drugs. The emergence of biofilms is on the increase much like the emergence of ‘superbug’ antibiotic resistant bacteria. In the treatment of nail fungus biofilms can block drug treatment. For antifungal drugs to work they need to target active fungal elements which are producing keratinases, proteolytic and other enzymes which result in the nail disease. Biofilms can contain both active and inactive dermaphytes. Those with low hyphal activity, termed the ’persisters’ are recalcitrant to drug therapy. Unfortunately, when conditions are right for them at a later point they can become active causing frustrating re-infection, even re-establishing new biofilms.
Podiatrists treating fungal nail infection need to be aware of fungal nail biofilms and understand that dematophytomas which may tick all the boxes for a low-grade infection could potentially be taxing to treat, with a high chance of re-infection if not treated as robustly as a high-grade infection The Lunula ‘cold’ laser has a 2- pronged approach in effectively treating fungal dermaphytes and tackling the problems posed by biofilms. The blue laser 405nm wavelength has an antimicrobial effect to tackle drug resistant biofilms and reach inactive dormant dermaphytes and spores. It is advisable to grade all possible dermatophytomas as high-grade infections to have at least 6 -8 laser sessions.
To really ensure success it would be prudent to try and get some antifungal drug directly into the source of infection by combining the Lunula with a Clearanail procedure. A combination treatment regime would help to ensure dormant biofilm trapped spores and dermaphytes are targeted to reduce risks of potential later re-infection.
If a patient is immuno-compromised or has other health conditions which could impede treatment effectiveness of a problematic dematophytoma, taking the infected nail plate off should be considered. In these cases, there could still be the presence of spores and dermaphytes in the nail folds, so a course of 4 Lunulas would ensure destruction of these as well as promoting accelerated healthy new nail growth and inhibit the chances of getting a new biofilm.
There are emerging new drugs e.g. efinaconazole which help to combat the problems associated with biofilms. The key is stop the attachment of micro-organisms to cells, to alter micro-organisms’ ability to synthesize extracellular matrix, and to allow better penetration of drugs into the extracellular matrix to kill the organism contained within the biofilm.
Whatever fungal nail treatment regime is chosen it is a process whereby there must be considerable patient compliance to adhere to all the post-treatment home care advice given, with attention given to address the presence of highly infectious spores. Patience is an essential requirement on both sides with realistic expectations established at the beginning of a treatment plan.
References:
- Costa-Orlandi CB et al. Fungal Biofilms and Ploymicrobial Diseases. J of Fungi 2017; 3-22
- Burkhart CN, Burkhart CG, Gupta AK. Dermatophytoma: recalcitrance to treatment because of existence of fungal biofilm. J Am Acad Dermatol. 2002 Oct;47(4):629-31.
- Richard A. Pollak, DPM, Boni E. Elewski, MD, Antonella Tosti, MD, and Tracey C. Vlahovic, DPM, FFPM, RCPS (Glasg) The Impact Of New Topical Antifungals On Onychomycosis Management
- Roberts DT, Evans EGV. Subungual dermatophytoma complicating dermatophyte onychomycosis. Br J Dermatol. 1998;138:189-90.
- Sullivan AN, Wang C, Cantrell WC, Elewski BE. Successful treatment of dermatophytomas with topical efinaconazole 10% solution. Abstract submitted to Winter Clinical Dermatology Conference 2017.
- Tracey Vlahovic, DPM, FFPM, RCPS (Glasg) When a patient Presents with Linear Streaks in a Nail. Podiatry Today Volume 28 – Issue 12 – December 2015, 20-24
- Update on Drugs and Drug News – February 2009 J Am Acad Dermatol 2002;47:629-31